Rheumatoid Arthritis (RA)
|
Definition:
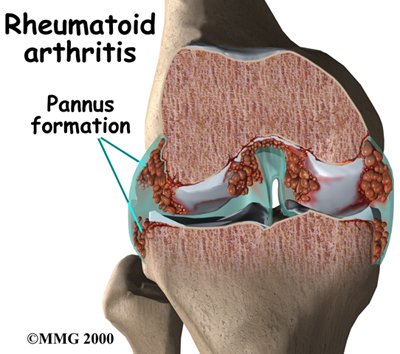
Rheumatoid Arthritis is a systemic autoimmune inflammatory disorder that attacks the synovial tissues around joints (Goodman). These attacks result in excessive proliferation of the synovial tissue and formation of granular tissues called pannus formations (Walther). This diagnosis is determined by examining three important factors (Goodman).
Risk factors: (Goodman, Walther)
Subjective: Symptoms will come on gradually and could take months to manifest completely during the first episode. The patient will complain of recent abnormal fatigue and generally achy muscles. Subsequent episodes will have a much more rapid onset of joint pain, swelling, and stiffness, due the inflammatory response occurring in the joint capsule (Goodman). Stiffness will be the worst in the morning and will last over 45 minutes after rising. A patient with RA in the knees is likely to have experienced this conditions in the feet and/or hand first (Goodman). Symptoms tend to be symmetrical because of the systemic nature of this condition. Also, symptoms may be aggravated by certain weather conditions as well as extreme temperatures. People with RA commonly experience unintentional weight loss as well as depressive symptoms (Walther). The following is a mnemonic for the word “serious” to help clinicians detect signs and symptoms associated with RA (Goodman). S = swelling in one or more joints E = early morning stiffness R = recurring pain and tenderness at the joint I = inability to move the joint normally O = obvious redness and warmth at the joint U = unexplained weight loss, fever, or weakness combined with joint pain S = symptoms that last for more than 2 weeks |
Objective:
Patients may present with a low grade fever during an episode. At the inflamed joint, the site will be swollen, red, warm, and tender to the touch. Range of motion of the affected joint is expected to be limited and painful (Goodman). Patients experiencing an acute flare up may walk with an antalgic gait with limited extension of the hip and knee. If the structural integrity of the joint has been compromised by the disease, this may be detectable to the clinician through passive accessory motions of the joint. Subcutaneous nodules may be palpable in the connective tissues surrounding the joint. A popliteal cyst is also commonly observed with RA in the knee (Walther). Intervention: Patients suffering from RA will likely be prescribed an immunosuppressive drug to help decrease the immune system for attacking the joint. Another class of drug is DMARDs, standing for disease-modifying antirheumatic drugs, which decrease both the symptoms and the rate of progression of the disease (Goodman). Patients should be educated on the pathophysiology of the disease and how to reduce their pain. Do not stretch the muscles surrounding the affected joint during the inflammatory period. Also during this time, resistance training and manual therapy should be avoided for the affected joint. During an inflammation episode, exercises should be restricted to gentle active and passive ROM. Stretching, strengthening, and mobilizations can be used when the patient is not experiencing an inflammatory episode. Patients with RA typically respond well to aquatic therapy for aerobic training and strengthening, but should also participate in land based activities (Walther). If your patient is not currently being seen by a rheumatologist and you suspect the onset of RA, a referral is warranted. If joint damages become excessive, surgeries and joint replacements may be considered. Assistive devices may eventually need to be considered for modified independent mobility (Walther). Tips for pain management: (Walther)
Prognosis: Without proper control by medications, RA can severely erode the articular surfaces of a joint within just two years (Goodman). Patients are likely to experience subluxations, contractures, and deformities in the affected joints (Walther). The overall decrease in functional activity leads to multiple comorbidities, and may decrease the longevity of independent life. |
References:
- Goodman, C.C., and T.E.K. Snyder. Differential Diagnosis for Physical Therapists Screening for Referral. 4. St. Louis: Saunders Elsevier, 2007. Print.
- Walther, H., and E. Palmer. "Rheumatoid Arthritis."CINAHL Rehabilitation Reference Center. EBSCO Publishing, 2011. Web. 2 Jul 2012. <http://web.ebscohost.com.p.atsu.edu/rrc/detail?sid=a56d20bf-1784-4bcf-8fca-dfae517c136d@sessionmgr13&vid=6&hid=9&bdata=JnNpdGU9cnJjLWxpdmU=
- Image from: http://www.google.com/imgres?hl=en&sa=X&rlz=1C1CHFX_enUS487US487&biw=1517&bih=725&tbm=isch&prmd=imvns&tbnid=Ed1st2edtletoM:&imgrefurl=http://www.orthopaedics.com.sg/conditions/joint-arthritis/rheumatoid-arthritis&docid=jFMMjn6h6xEUbM&imgurl=http://www.orthopaedics.com.sg/wp/wp-content/uploads/2011/07/rheumatoid-arthritis.jpg&w=400&h=354&ei=KuLsT7e-F-Ha0QHg-pDKDQ&zoom=1&iact=rc&dur=507&sig=118100015442533972417&page=1&tbnh=156&tbnw=176&&ndsp=19&ved=1t:429,r:14,s:0,i:186&tx=71&ty=78