Anterior Cruciate Ligament (ACL) Tear/Sprain
Definition:
The ACL is a passive stabilizer of the knee and guides motion between the tibia and the femur, as well as preventing excessive anterior motion (Fleming, et al.). If the motion is excessive or mechanically disrupted the risk of tearing a ligament is higher (Dutton). The ACL is the primary restraint to anterior translation and reinforces the MCL and controls rotation of the tibia on the femur towards the end of extension (Dutton). Posterolateral portion of the ligament is taut when the knee is in extension, it is the most commonly injured portion (Dutton).
Subjective:
Objective:
Intervention:
The ACL is a passive stabilizer of the knee and guides motion between the tibia and the femur, as well as preventing excessive anterior motion (Fleming, et al.). If the motion is excessive or mechanically disrupted the risk of tearing a ligament is higher (Dutton). The ACL is the primary restraint to anterior translation and reinforces the MCL and controls rotation of the tibia on the femur towards the end of extension (Dutton). Posterolateral portion of the ligament is taut when the knee is in extension, it is the most commonly injured portion (Dutton).
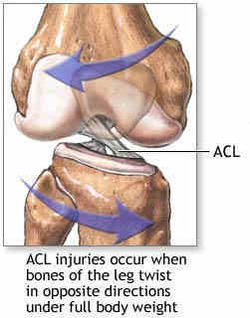
- Mechanism of Injury: The most common contact mechanism is a blow to the lateral side of the knee resulting in a valgus force to the knee, this can also lead to medial collateral ligament injury and medial meniscus injury often called “terrible triad” (Kisner & Colby). The most common non contact mechanism is a rotation mechanism in which the tibia is externally rotation with slight knee flexion and a planted foot. The second most common mechanism is forceful hyperextension of the knee (Kisner & Colby).
- Categorized as grade I, II, III injuries, ranging from overstretched fibers to complete ligament rupture (Dutton).
- A narrow intercondylar notch, weak ACL, joint laxiy, LE malalignment can lead to an increase in injuries to the ACL (Dutton).
Subjective:
- Feel or hear a “pop” sensation
- Mild to moderate aching pain
- Instability because of the knee buckling or a feeling of the knee giving way
- May complain of swelling (Foster, et al.).
- Possible discomfort, stiffness, numbness, tingling, and possible contusions
Objective:
- Impaired gait
- Muscle girth is likely to be different compared to the uninjured leg due to swelling or possible atrophy depending on the time frame.
- Valgus stress test (gapping and stressing the medial collateral ligament)
- Lachmans: expect anterior translation of the tibia because the ACL is absent to check it.
- Anterior Drawer: patient in supine with hips flexed and knees at 90 degrees, sit on patient's feet while grasping tibia and pulling forward. Excessive displacement is a positive test.
- Pivot and shift determines rotational stability of the knee.
- Bollotman test: push the patella against the trochlear groove, the patella will rebound if there is effusion.
- KT 1000/2000 Arthrometer-Testing anterior tibial translation relative to the femur under multiple applied forces, a laxity test looking at knee stability (Foster, et al & Dutton).
Intervention:
- Operative reconstruction.
- Intervention varies from maximum protection phase to moderate protection phase to minimal protection phase.
- Pre rehabilitation (before surgical intervention) is recommended.
- Conservation treatment is also an option dependent on patient.
References:
- Dutton M. Orthopaedic Examination, Evaluation, and Intervention. 2nd ed: The McGraw-Hill Companies, Inc.; 2008.
- Fleming BC, Hulstyn MJ, Oksendahl HL, Fadale PD. Ligament injury, reconstruction, and osteoarthritis. Curr Opin Orthop. 2005;16:354–362.
- Kisner, Carolyn & Colby, Lynn A. Therapeutic Exercise 5th Edition. Foundations and Techniques. 2007; pp 725-735.
- Foster, Timothy E., Wolfe, Brian L., Ryan, Scott., Silvestri, Lorenzo and Kaye, Elizabeth Krall. Does the Graft Source Really Matter in the Outcome of Patients Undergoing Anterior Cruciate Ligament Reconstruction? : An Evaluation of Autograft Versus Allograft Reconstruction Results: A Systematic Review. Am J Sports Med. 2010 38: 189.
- Image: http://www.musclegeeks.com/2012/02/acl-prevention-and-basketball-does-your-training-program-have-the-requirements/
